When antibiotics stopped working, these viruses saved a girl's life
Phage therapy is attracting renewed interest in treating highly resistant infections
When Isabelle Carnell-Holdaway was discharged from the Great Ormond Street Hospital in London in 2017, her prognosis was grim. The 15-year-old had undergone a double-lung transplant seven months earlier as a result of her cystic fibrosis, a degenerative condition she was born with. Although there had not been any complications with the surgery, Carnell-Holdaway's immune system was suppressed, and an opportunistic drug-resistant infection had taken hold at the surgical site. Carnell-Holdaway was taken off of most antibiotics after she experienced severe side effects, including liver failure, and she left the hospital with a palliative care plan in place.
Thousands of miles away, researchers at the University of Pittsburgh were racing to refine a therapy that would ultimately save the teenager's life. The results of Carnell-Holdaway's treatment were published recently in the journal Nature Medicine; now, the treatment is gaining renewed interest, with some even going as far as to call its effects "miraculous."
The treatment, called phage therapy, has existed for a century, and its underlying concept is elegant: Co-opt viruses that naturally infect bacteria to treat infections while ignoring human host cells. The use of these viruses, known as bacteriophages or phages for short, proliferated in the Soviet Union in the early 20th century in the absence of antibiotics, but the practice has only recently been rediscovered. It is gaining popularity in the United States and Europe, where it is being tested as a way to treat everything from burns to urinary tract infections.
As a last-ditch option, one of Carnell-Holdaway's doctors reached out to Graham Hatfull, a professor at the University of Pittsburgh whose lab studies bacteriophages that infect the tuberculosis family of bacteria. Carnell-Holdaway was infected with a member of this bacteria family, which is known to target immunocompromised patients, and Hatfull and his team searched through a library of over 10,000 different phages to find the ones that would attack her strain the best. After identifying three that could infect the bacterium effectively, the researchers had one more roadblock to surmount: One of the phages was programmed to infect, but not kill the bacterium. This behavior is known as the lysogenic cycle, in contrast to the lytic cycle in which a virus copies itself before bursting out of its host cell and destroying it.
To address the issue, Hatfull's team genetically engineered the misbehaving phage to express lytic behavior. This was the first time that an engineered phage has been used in a clinical setting. After conducting the necessary quality control experiments and obtaining regulatory permission to ship the phages from the U.S. to the U.K., the team sent off the three-phage cocktail to Carnell-Holdaway's doctors, about six months after they had been first contacted.
But while time pressures were ever-present in the back of the researchers' minds, Hatfull told me in an interview that the work began as a purely hypothetical exercise — seeing if their library contained the right phages — and only later morphed into a treatment Carnell-Holdaway might actually receive.
.jpg)
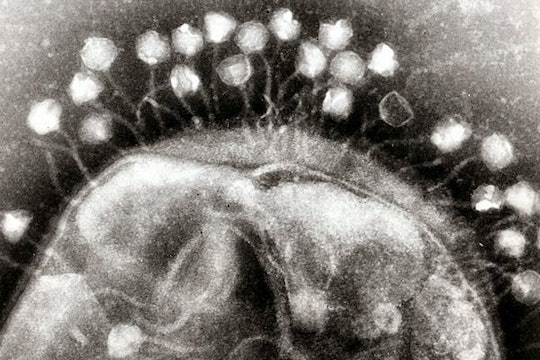
Microscope image of a Mycobacterium, a member of the family that causes tuberculosis
Carnell-Holdaway started to show improvement within weeks of beginning intravenous treatment with the phages every 12 hours — skin lesions caused by the infection started to clear up, her lung function improved and she gained weight. Still, since her treatment was not conducted like an experiment, it is impossible to be 100% certain that the phage therapy caused her recovery.
After nine days of monitoring in the hospital, Carnell-Holdaway had not reported any adverse reactions to the phages, an outcome "that obviously came as a not insubstantial relief to all of us," Hatfull says. When her doctors decided to discharge her from the hospital again, they were optimistic about her chances of recovery.
Even with the long history of phage therapy in Eastern Europe, this was the first recorded instance of both a genetically engineered phage used clinically and an infection in the tuberculosis family being treated with phages.
"We're in uncharted territory," Hatfull says.
But that has not stopped researchers and media outlets alike from speculating that phage therapy may one day replace antibiotics as first-line treatments of drug-resistant infections. This kind of "silver bullet" thinking is misplaced, says Hatfull, though he does think phage therapy will likely be the solution to some types of highly resistant infections.
The story of Carnell-Holdaway's treatment is a case study into the difficulties facing widespread clinical implementation of phage therapy and a potential roadmap to solving them.

Implementing phage therapy is challenging, but now we have a roadmap for dealing with some of the associated problems
Luis Melendez on Unsplash.
One problem is the phage's specificity. From an evolutionary standpoint, it makes sense that a highly specialized phage would perform better than a jack of all trades. This has resulted in highly specific phages that are best at infecting substrains within strains: The three phages Hatfull's team identified as candidates to treat Carnell-Holdaway's infection were not effective against other isolates of the same bacterium. At the same time, only a tiny fraction of the estimated ten nonillion, or 10³¹, phages have been discovered and categorized in a library. And once these massive libraries are established, there needs to be infrastructure in place for quickly and cheaply determining the few relevant phages for any specific infection.
Programs like SEA-PHAGES, run by Hatfull's lab and the Howard Hughes Medical Institute in the U.S., are trying to address the latter challenge using crowdsourcing. SEA-PHAGES trains undergraduate researchers from more than 100 colleges and universities around the country to discover and sequence phages over the course of two semesters, and the program will soon reach 3,000 sequenced phage genomes.
Carnell-Holdaway will soon reach a milestone, too: One year of continuous phage treatment. During that time, she has returned to a normal life and is busy with schoolwork and A-levels. Hatfull says there is no telling how long Carnell-Holdaway will remain on treatment, nor whether the phages will keep the infection at bay permanently.
Nevertheless, future work to engineer and refine phage technology offers great promise for the treatment of disease. "It's really exciting," Hatfull says. "We love this idea of being able to creatively think about how you could fine-tune what you might think of otherwise as a relatively crude technology, and the potential is substantial."