Penn State University
Lasers can help us detect viruses faster than typical medical tests
Laser beams vibrate proteins in unique ways
To detect a virus, you need to already know intimate details about it. You need to design a test particular to that virus: one that finds and copies only a specific, identifying piece of its genetic material.
But Mauricio Terrones and his collaborators at Penn State University think they’ve found a better way. Described recently in Proceedings of the National Academy of Sciences, their method, VIRRION, may be a faster and more versatile diagnostic tool than the conventional polymerase chain reaction (PCR) virus tests.
PCR works by making millions of copies of DNA or RNA to enhance the detection of viruses, including the novel coronavirus, SARS-CoV-2. The ongoing pandemic has led to advances in the speed of PCR tests. But the test is based on biochemical processes that occur at specific temperatures, so researchers can't process tests any faster than the several hours it takes to heat and cool the sample many times. Not only that, a PCR test will only recognize the virus that it was specifically designed to test, so a new test must be developed and disseminated each time a new virus pops up. The delay between the emergence of a virus and the availability of tests can lead to devastating consequences.
VIRRION addresses both of these issues. Preliminary tests on three different viruses show that it can identify a virus with 70-90 percent accuracy within a few minutes of receiving a sample.
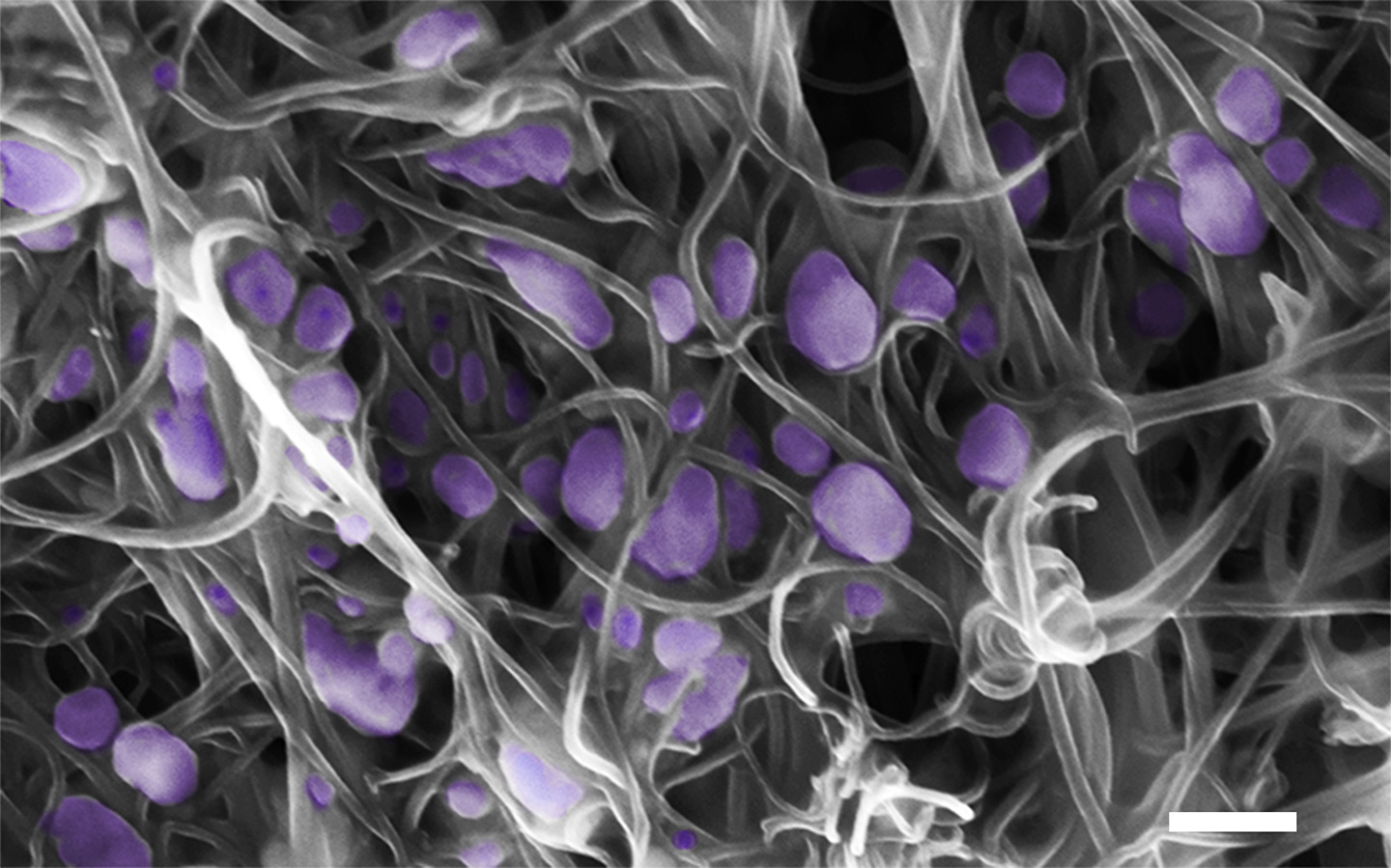
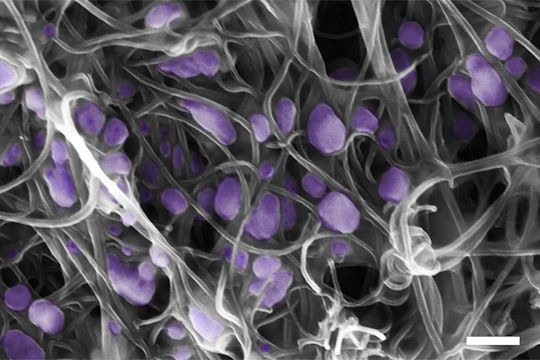
Viruses (purple) caught in a carbon nanotube "forest"
Penn State University
The first step of the VIRRION method is to enrich the sample, or increase concentration of the virus, making it easier to detect the virus. There are two ways to do this: either increasing the number of virus particles, or decreasing the number of unwanted particles. Proponents of PCR opt to amplify the signal, making copies of the viral DNA or RNA. But VIRRION takes the alternative approach, increasing the concentration of virus particles by eliminating the unwanted junk in the sample. To do this, the researchers filter the sample through a cartridge containing hundreds of thin, carbon nanotubes.
Imagine a forest, says Terrones, where the deeper into the forest you travel, the denser the trees become. Eventually, the forest is so dense that it's impossible to run between the trees. As the virus travels through the cartridge, it moves through a progressively thicker and thicker forest of carbon nanotubes. Eventually the virus gets caught between two of the tubes, and all of the smaller junk passes through.
After capturing the virus particles, Terrones and his team shine a laser on the sample, using a technique called Raman spectroscopy to analyze the structure of the virus.
This Raman technique is based on the notion that vibrations or sound waves in a material give us information about the structure of that material. Knock on a table or desk or wall nearby. You can probably guess what material something is by the sound it makes. A metal desk might resound in a high-pitched ring, while the wooden kitchen table will eke out a dull, staccato, “thump.” You can tell what the material is because your ear is remarkably good at analyzing the spectrum of sounds — that is, the combinations of different frequencies of sound. And the sounds that a material emits is a function of the structure of the material itself.

Terrones adjusting mirror for laser set up
Nate Follmer (Penn State University)
Researchers can do the same thing to viruses with Raman spectroscopy by "knocking" the virus, with light instead of their knuckles. The light causes proteins on the surface of the virus to vibrate. Scientists can then analyze the spectrum of light that bounces off of the virus and learn how the virus is vibrating, and consequently about its structure. And, as it turns out, each virus in this study has a different surface structure, so the Raman spectrum serves as a fingerprint that uniquely identifies a specific virus.
After researchers get a fingerprint, they use a machine learning algorithm to match it to a database to discover the viral culprit. Terrones says that provided they have a good database and machine learning algorithm, they could even identify two different viruses within a single sample.
Terrones sees VIRRION as a technique to potentially complement — not replace — PCR. The accuracies of PCR tests vary, but most of the best tests perform better than VIRRION. While their method may be improved upon with time, the real selling point is the promise of rapid results. Terrones thinks it may find a place in screenings, where if somebody tests positive in a VIRRION test, conventional methods can be used afterward on the same sample to verify the result — though this would only be useful for verifying positive cases, not for addressing potential false negatives.
Since this is such a new technique, it likely won’t be able to contribute to quelling the current pandemic. However, some experts suggest that SARS-CoV-2 might continue to rear its head long after the pandemic, perhaps becoming a seasonal virus like the flu or cold. Terrones wants to be ready for this eventuality. He and his team have started testing their technique on animal coronaviruses, with a preliminary detection accuracy of 99%. They aim to eventually move to human coronaviruses, including SARS-CoV-2.
