How your immune system can give you narcolepsy
New research could lead to easier diagnoses of this rare sleep disorder
Narcolepsy is a rare neurological disorder that disrupts the brain’s regulation of sleep and wake. It is often portrayed comically in movies and television; think that 2015 episode of The Simpsons, when Homer’s chuckling, deep-voiced doctor diagnoses him after a mishap at the nuclear power plant. But the condition is no joke, especially for children. People with narcolepsy can have dreams that continue after waking, called hypnogogic hallucinations, which are sometimes misdiagnosed as schizophrenia. And one form of the disorder, type 1 narcolepsy, causes sudden muscle weakness, brought on by strong emotions or stress. In short, it can be a debilitating condition.
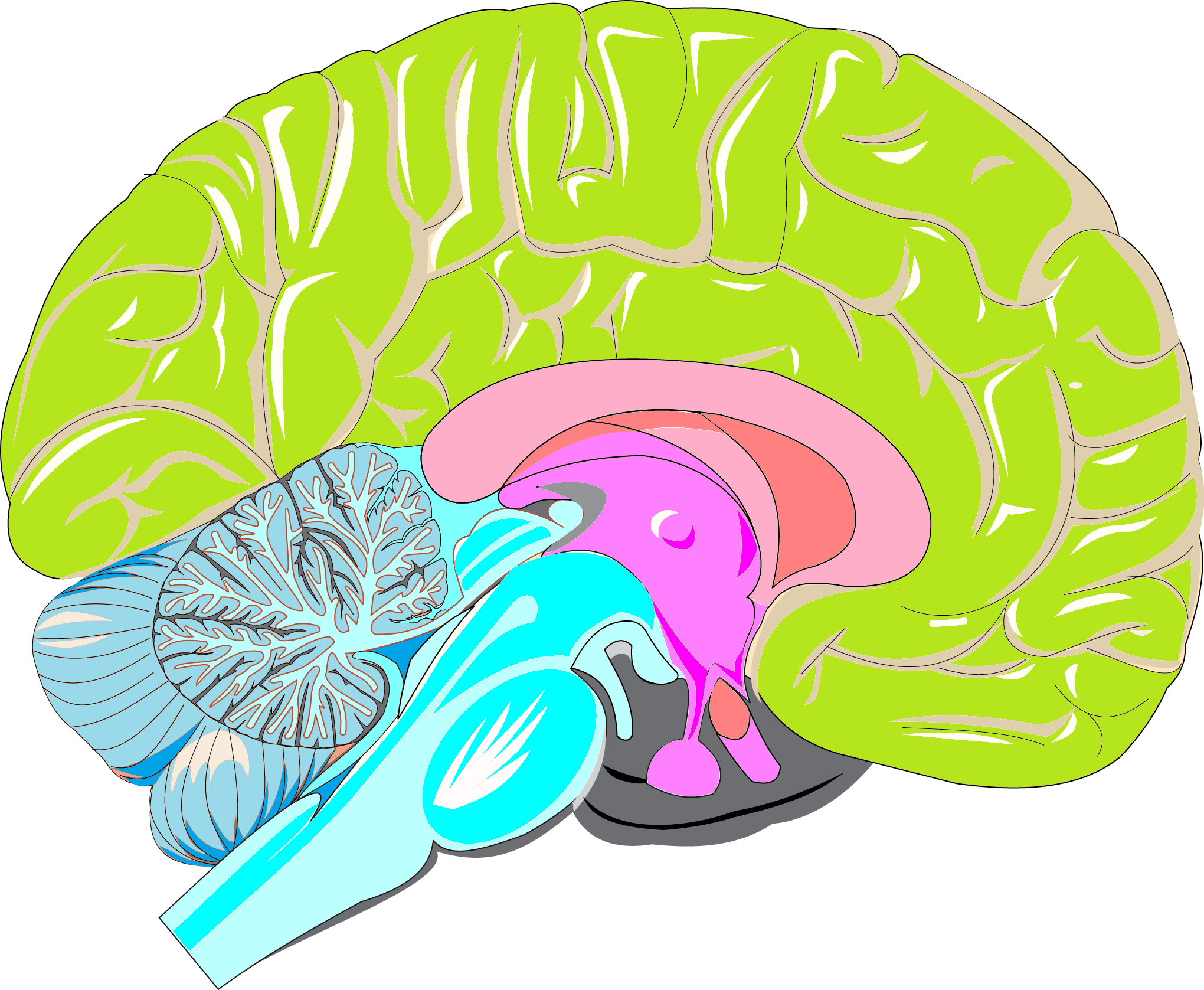
The home of narcolepsy
Neurologists have suspected for years that narcolepsy results from an autoimmune attack on the brain. But no one had been able to demonstrate firm evidence for the theory. That's why it was big news when in September, researchers from Switzerland reported in Nature that they could detect treacherous T-cells—immune cells that rally a response to intruders—in the blood of people with narcolepsy. In people with the disorder, the paper suggested, these cells might identify a protein produced within the brain, and then mistakenly direct the immune system to attack it. Another recent paper from Stanford suggests that influenza virus could be a trigger for this destructive confusion.
These major advances illuminate the origin of narcolepsy, and are expected to make diagnosis easier. They have also spurred proposals for intervention that could modify the course of the disease. Taken together, the two papers show that Type 1 narcolepsy is analogous to Type 1 diabetes. In diabetes, the immune system eliminates cells in the pancreas that secrete insulin. In Type 1 narcolepsy, what goes missing are cells in the brain that produce hypocretin, a neuropeptide which usually keeps people awake and alert. When people develop narcolepsy, something—a viral infection, perhaps—triggers the immune system, making it go haywire and start to attack the neurons that make hypocretin.
Neurologists have thought that type 1 narcolepsy could have an autoimmune basis since the 1980s, because the strongest genetic risk factor is a variant of an HLA gene—and HLA genes encode proteins that guide T cells’ activation. However, way more people have the HLA risk factors (more than 20 percent of some population groups) than type 1 narcolepsy itself, which is estimated to occur in 1 in 2,000 people. A mechanistic link has been difficult to detect; it isn't convenient to view someone's brain under a microscope when symptoms begin to appear.
At the 7th International Symposium on Narcolepsy this fall, Claudio Bassetti, chair of neurology at Bern’s University Hospital, said that he had been trying to convince immunologists to work on narcolepsy for years, before finally collaborating with Federica Sallusto, at the University of Italian Switzerland.
The scientists decided to design an experiment that amplified the small numbers of T-cells present in narcolepsy patients’ blood. The researchers were then able to identify both hypocretin-specific CD4+ (“helper”) and CD8+ (“killer”) T-cells in the patients' samples. These cells were much less abundant, or absent altogether, in samples from people without narcolepsy.
These T-cells "can cause inflammation leading to neuronal damage or even kill hypocretin-producing neurons,” Sallusto said in a statement. “By blocking them at early stages, it may be possible to limit neuronal loss and prevent progression of the disease.”
Attempts to do so have already been tried on a limited scale. Immune intervention is not necessarily expected to help people living with the disorder for a long time, because it can't restore hypocretin-producing neurons that have already been lost. But weeks, or even months, after symptom onset, it might be possible to save some endangered neurons and reduce symptom severity. This would make early diagnosis—which can be challenging in adults—even more critical.
Fifteen years ago, Michel Lecendreux, a child psychiatrist and sleep researcher from Paris, led a team that tried treating new-onset type 1 narcolepsy with a blend of antibodies (intravenous immunoglobulin or IVIG). Following this fall's discoveries, instead of IVIG, narcolepsy researchers are discussing borrowing medications for multiple sclerosis, which could stall the advance of T cells into the brain. At the symposium, Lecendreux suggested that “the clock is ticking” for patients recently diagnosed, but noted a lack of consensus on if the next step should be a randomized controlled trial, or smaller open label studies, in which everyone knows what the patient is receiving.
What's been tested so far with IVIG and other drugs is a "shotgun approach" to immunosuppression, said Mark Patterson, president of the board of directors for Narcolepsy Network, a patient advocacy organization.
"As a scientist, I would love to see the result of a randomized trial," said Patterson, who attended the symposium. "But as a pediatrician and a parent of a child with narcolepsy, I would push for open label trials. I would be hesitant to target a specific pathway at this point."
One outstanding question is how influenza, either due to vaccinations or viral infection, may cause the disease in people with genetic risk. Around the time of the 2009-2010 H1N1 pandemic flu outbreak, an increased rate of narcolepsy in flu patients was reported from China, and also in some countries where a particular flu vaccine (Pandemrix) was used. The effect was seen only in some European countries, and a similar vaccine (Arepanrix) did not lead to the same issues in Canada.
.jpg)
Another reason to get a flu shot
The Stanford paper published in December, from Emmanuel Mignot's lab, partly explains the flu connection. Mignot, in his own explanation of his team's paper, explicitly takes a pro-vaccine stance and pairs it with a photo of hand-washing. The new paper is actually a follow up to a previous effort that was retracted in 2014, after some of the data could not be reproduced. The new one adds more molecular details and genetic analysis.
Both the Stanford and Swiss papers identify troublesome T-cells that target hypocretin, but they diverge in a few ways. Unlike some of the narcolepsy cases in the Stanford paper, none of the participants in the Swiss paper were connected with Pandemrix. Also, in the Swiss paper, the regions of hypocretin recognized by T-cells are spread out along the entire protein. In contrast, the Stanford researchers show T cells recognizing only a couple sections of the protein.
The Stanford team has suggested the T cells they identified reveal an earlier stage of autoimmunity. According to them, autoimmunity develops through molecular mimicry. Part of the 2009 H1N1 flu virus, which was used in the Pandemrix vaccine, looks like a stretch of hypocretin. Either infection with the virus, or vaccination, activates T-cells that recognize that bit of protein. Once the immune system gathers momentum, it starts recruiting T-cells that recognize and attack other parts of hypocretin, and subtly damaging the brain.

Allan Lasser
Researchers still have a long way to go before they fully understand type 1 narcolepsy. Plenty of people who have the HLA genes avoid developing narcolepsy, even if they are infected by flu or vaccinated. At the symposium, researchers agreed that the available evidence suggests a “multi-hit hypothesis”. In this scenario, there is pre-existing inflammation in the brain, followed by a second hit—like a case of the flu—that prompts the immune system to attack hypocretin-producing cells. Even without all the details, the narcolepsy field has turned a corner toward insights that could help people with this puzzling condition.


Just wanted to point out this rather disturbing and well done paper from MGH showing that sleep fragmentation messes up hypocretin-producing cells (in mice), with effects on CVD.
And Jerry Siegel and company’s finding that opiates increase hypocretin-producing cells, which was the other mind-blower at the narcolepsy meeting in September.